A stool sample test can detect infections, inflammation, blood in the stool, and problems with digestion or absorption. In the NHS, stool tests are primarily used to rule out serious conditions such as infections, inflammatory bowel disease, or bowel cancer.
Functional Medicine private stool tests can also assess the gut microbiome, yeast such as Candida, and markers like zonulin, which relates to gut barrier function.
If you are experiencing symptoms such as bloating, diarrhoea, constipation, abdominal pain, or changes in bowel habits, a stool test can help identify potential underlying causes.
In this article we will discuss the main differences between a NHS stool test and a private Gut Health test.
Specifically we will cover:
- What does a stool test show?
- What does a stool sample test for?
- What can a stool test detect?
- What do stool samples check for?
- Exactly what stool tests detect and the types of stool tests
- The difference between NHS stool tests vs private gut health tests
Infection
What Can be detected in a Stool Sample on the NHS ?
1.Infections and Bacteria found in a stool sample
An NHS stool test can be helpful to screen for bacteria.
Stool sample tests can detect bacterial infections such as Campylobacter, Salmonella, Shigella, and certain strains of E. coli, as well as Clostridioides difficile, which is often associated with recent antibiotic use.
Bacterial pathogens are a frequent cause of acute gastrointestinal symptoms.
Common strains of bacteria that can be examined include:
- Campylobacter – the leading cause of bacterial diarrhoea in the UK, often associated with undercooked poultry
- Salmonella – typically linked to contaminated eggs, poultry, or processed foods
- Shigella – spread through contaminated food or water, particularly in areas with poor hygiene
- Certain strains of Escherichia coli – particularly those associated with undercooked meat or contaminated produce.
- Clostridioides difficile (commonly known as C. diff). This bacterium can cause severe inflammation of the bowel. It can occur in patients who have taken antibiotics.
- Helicobacter Pylori can also be tested in a stool test.
In some cases, particularly following foreign travel or persistent symptoms, stool tests may also be used to detect parasites such as Giardia or Entamoeba histolytica.
2. Inflammation
Stool tests can also measure markers of inflammation, most commonly calprotectin. This helps distinguish between inflammatory bowel conditions such as Crohn’s disease or ulcerative colitis, and non-inflammatory conditions such as IBS.
A normal calprotectin level makes inflammatory bowel disease much less likely, whereas elevated levels may indicate inflammation that requires further investigation.
3. Blood in the Stool- Cancer in a stool test
Your GP may request a FIT (Faecal Immunochemical Test), which detects small amounts of blood in the stool that are not visible to the naked eye.
This test is commonly used to help rule out conditions such as bowel polyps or colorectal cancer, particularly if you have symptoms like unexplained weight loss, persistent changes in bowel habits, or anaemia.
4. Digestive Function
Some stool tests can also provide insight into how well you are digesting and absorbing food. For example, pancreatic elastase is used to assess pancreatic function.
Low pancreatic elastase may suggest impaired digestion of fats and proteins, which can contribute to bloating, nutrient deficiencies, and changes in stool consistency such as pale, greasy, or floating stools.
What Parasites Does an NHS Stool Test Check For?
NHS stool tests can detect certain parasites, but testing is usually only done if there is a clinical reason, such as persistent diarrhoea or recent travel.
The most commonly tested parasites include:
- Giardia
- Cryptosporidium
- Entamoeba histolytica
These infections are typically linked to contaminated food or water and can cause symptoms such as diarrhoea, bloating, and abdominal pain.
What Symptoms Can a Stool Test Help Investigate?
Stool tests are commonly used when someone experiences:
- Diarrhoea (especially persistent or severe)
- Bloating and excessive gas
- Abdominal pain or cramping
- Changes in bowel habits (constipation or urgency)
- Blood or mucus in the stool
- Unexplained weight loss
- Fatigue linked to digestive issues
Can a Stool Test Diagnose IBS?
A stool test cannot diagnose IBS directly. Instead, it is used to rule out other causes such as infection, inflammation, or blood in the stool. IBS is typically diagnosed based on symptoms once these conditions have been excluded.
What types of Stool Tests are Available in Functional Medicine?
If your NHS stool test has come back “normal”, this can be reassuring from a medical perspective, however it does not always explain why symptoms such as bloating, or irregular bowel movements are occurring.
If you are still experiencing symptoms, there are different types of stool test that are available. Functional medicine stool testing will look at additional markers that may have not been assessed by the NHS and may be able to help in understanding the root cause of your symptoms.
What Private Gut Health Tests Can Assess
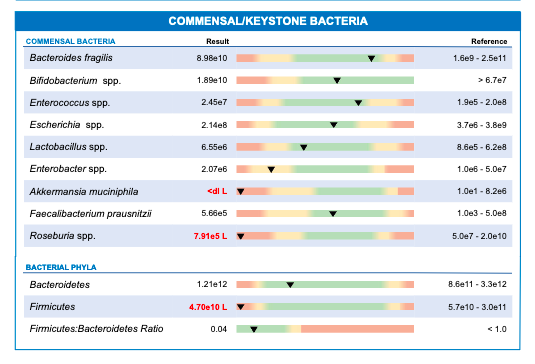
1. Gut Bacteria Balance (Microbiome)
Unlike standard NHS testing, gut health tests also known as comprehensive stool tests assess:
- Levels of beneficial bacteria
- Overgrowth of opportunistic organisms (including bacteria and yeast)/candida
- Overall microbial balance (known as dysbiosis)
This is particularly helpful if you have IBS-type symptoms.
The gut contains a wide range of beneficial bacteria, particularly Lactobacillus and Bifidobacterium, which play a central role in maintaining a healthy gut environment.
They support digestion and are involved in the breakdown and absorption of nutrients, especially fibre and certain vitamins.
These microbes also help protect against the overgrowth of harmful organisms and contribute to the normal functioning of the immune system within the gut.
When levels of beneficial bacteria are reduced, this balance can be disrupted, which in some cases may contribute to opportunistic strains of yeast and bacteria overgrowing and symptoms such as bloating, digestive discomfort, and increased sensitivity to foods.
2. Overgrowth of Opportunistic Organisms
In addition to beneficial bacteria, the private gut health test can also detect contains organisms known as opportunistic microbes- yeast or bacteria.
These are normally present in small amounts and coexist without causing harm. However, when the balance of the microbiome is disrupted, these organisms can increase in number and begin to contribute to symptoms. including gas, bloating, changes in bowel habits, and general gut irritation.
Examples include certain Streptococcus species, Enterococcus, and other opportunistic bacteria or yeast such as Candida.
3. Overall Microbial Balance (Dysbiosis)
Rather than focusing on a single organism, these tests assess the overall balance of the microbiome.
The gut microbiome functions like an ecosystem.
When the balance of bacteria in the gut is disrupted (often called dysbiosis), it can lead to increased fermentation of food, which produces gas and bloating. At the same time, it can affect how the gut moves (motility), slow things down or speed them up, and make the gut lining more sensitive. This can trigger symptoms like discomfort, food reactions, and IBS-type symptoms.
When this balance is disrupted, it can affect:
- Digestion
- Gut motility
- Immune signalling
- Sensitivity to foods
4. Digestive Function
Markers such as pancreatic elastase provide insight into how well you are digesting and breaking down food. Although this marker can be conducted on NHS stool tests, in my experience it is not routinely carried out.
When levels are low, it can suggest that fats and proteins are not being properly digested, which may lead to reduced nutrient absorption.
This can often show up as symptoms such as bloating, fatty or floating stools, and general digestive discomfort, as the body is not fully breaking down and absorbing what you eat.
5. Gut Immune Function
Secretory IgA (sIgA) reflects how active your gut immune system is and how well it is protecting you. When levels are low, it can suggest reduced defence, meaning the gut may be more vulnerable to microbes such as bacteria or yeast.
On the other hand, high levels can indicate immune activation, suggesting the body is responding to something in the gut. Overall, this marker helps us understand how your immune system is interacting with and responding to the microbes in your digestive system.
6. Inflammation Markers
Some comprehensive tests also include markers of inflammation. such as Calprotectin.
As previously mentioned this marker is also carried out routinely by the NHS and will distinguish between inflammatory bowel conditions and non-inflammatory conditions such as IBS.
7. Gut Barrier Markers
Markers such as zonulin may be included in some advanced stool tests and are used to give an indication of gut barrier function. The gut lining acts as a protective barrier, allowing nutrients to pass through while keeping unwanted substances such as toxins, bacteria, and undigested food particles out of the bloodstream.
When zonulin levels are elevated, it may suggest increased intestinal permeability, often referred to as “leaky gut.” This means the barrier is not functioning as effectively as it should, which can allow substances to pass through more easily and potentially trigger immune responses, inflammation, and food sensitivities.
8. Parasites in Comprehensive Stool Testing
Unlike standard NHS stool tests, which typically only screen for a few parasites comprehensive stool tests used in functional medicine use advanced methods such as PCR (DNA-based testing) to detect a wider range of parasites, including organisms that may be missed on routine testing.
This can include parasites such as Giardia, Blastocystis hominis, Dientamoeba fragilis, and other protozoa, as well as evidence of helminths (worms) in some cases.
The benefit of these tests do not just identify whether a parasite is present — they can also provide context. For example, they may indicate levels of colonisation, co-existing imbalances in the gut microbiome, and markers of inflammation or immune response. This helps build a more complete picture of how the parasite may be interacting with the host.
This is particularly relevant in individuals with ongoing symptoms such as bloating, gas, diarrhoea, fatigue, or IBS-type symptoms, especially when standard stool tests have come back normal. In some cases, parasites may be present without causing symptoms, while in others they may contribute to gut irritation, altered bowel habits, and disruption of the microbiome.
Key Takeaway
If your NHS stool test is normal but symptoms persist, a more detailed stool test may help provide: Standard stool tests are designed to detect clear disease.
Private Comprehensive stool testing, however, can help identify:
- Leaky gut
- Candida
- Broader range of Parasites/Worms
- Bacteria including Helicobacter Pylori and Salmonella and E.coli
- Inflammation
If you have been told your stool test results are “normal” but you are still struggling with symptoms, there may be an underlying imbalance that has not yet been identified.
Advanced gut testing such as GI-MAP with Zonulin can be ordered through our website
Alternatively if you are experiencing ongoing digestive symptoms and would like a more in-depth discussion, we offer 1-hour consultations at our sister clinic ibs-solutions.co.uk
We can help identify the underlying causes and provide a personalised plan to support your recovery.
We can help with candida, SIBO, leaky gut, food intolerances and IBS.
NHS vs Functional Medicine Stool Tests: What’s the Difference?
If you are wondering what the difference between NHS and private Gut Health tests is- please see this comparison table below:
| Feature | NHS Stool Test (GP) | Functional Medicine Stool Test |
|---|---|---|
| Main Purpose | Rule out serious disease or infection | Understand underlying causes of symptoms of IBS |
| Infections (bacteria, parasites) | ✔ Yes | ✔ Yes (often more sensitive) |
| Inflammation (e.g. calprotectin) | ✔ Yes | ✔ Yes |
| Blood in stool (FIT test) | ✔ Yes | ❌ Not typically included |
| Gut bacteria balance (microbiome) | ❌ No | ✔ Yes |
| Beneficial bacteria (e.g. Lactobacillus, Bifidobacterium) | ❌ No | ✔ Yes |
| Opportunistic bacteria / dysbiosis | ❌ No | ✔ Yes |
| Yeast / Candida | ❌ No (unless severe) | ✔ Yes |
| Digestive function (e.g. elastase) | ⚠️ Sometimes | ✔ Yes |
| Gut immune markers (e.g. sIgA) | ❌ No | ✔ Yes |
| Gut barrier markers (e.g. zonulin) | ❌ No | ✔ Yes |
| Best for | Acute symptoms, red flags, such as blood, weight loss, ruling out disease | Ongoing symptoms, IBS, bloating, food sensitivities, irregular bowels |
| Limitations | May be “normal” despite symptoms | Not designed to diagnose serious disease |
Author – Victoria Tyler BSc Hons MBANT
Victoria Tyler owns and runs two busy clinics : Nutrition and Vitality and the IBS and Gut Disorder Clinic.
Nutrition and Vitality, along with the IBS and Gut Disorder Clinic, were founded with the goal of helping patients alleviate IBS symptoms by uncovering and addressing the root causes of their digestive issues.
As a Registered Nutritional Therapist, Victoria holds a BSc (Hons) in Nutritional Therapy and has trained with the Institute of Functional Medicine. She is also accredited by BANT and CNHC.
Before transitioning into health, Victoria earned a degree in Economics and an MBA, working with corporations including Canon and Vodafone. However, her own health challenges led her to pursue a career in Nutritional Therapy.
With a passion for learning, Victoria is committed to staying at the forefront of Functional Medicine. She helps patients manage IBS and other digestive disorders, including SIBO, Candida, and IBD, by identifying and addressing their root causes.
Victoria strongly believes that every symptom has an underlying cause, and there is always a solution to every health condition. To learn more, or to see patient reviews, visit Victoria’s profile on Google.
DISCLAIMER: The information provided in this article is intended for general informational purposes only and should not be construed as medical advice, diagnosis, or treatment. The products and methods mentioned are not a substitute for professional medical advice from a trained healthcare specialist. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. Use of the information and products discussed is at your own risk.







